(Guest post by Dr. Eric Rhoden, PT, DPT)
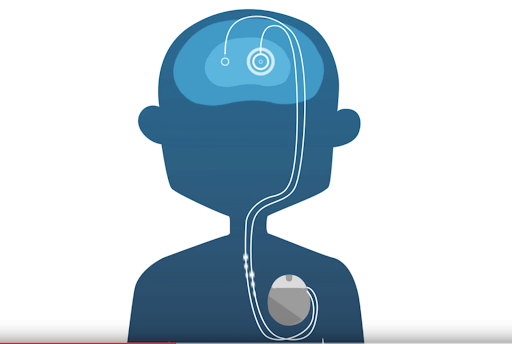
Until recently deep brain stimulation (DBS) for Parkinson’s Disease has been a monopolized industry run and operated by Medtronic, who has produced an amazing device that has changed countless lives. However, technology has developed at a rapid pace over the last year, and now there are more options to be aware of when you’re considering DBS surgery.
What do you need to know about Deep Brain Stimulation? (photo credit: Boston Scientific)
Currently in the US there are three companies that offer DBS:
Medtronic
Boston Scientific
Abbott
Each has unique technology they believe gives their patient’s the best outcomes. In this article, we’ll break down each system to explain the most important similarities and differences.
Looking for a great overview of DBS? Check out Part I of this series:
The Who, What, Where, When and Why of Deep Brain Stimulation for Parkinson’s Disease
Deep Brain Stimulation For Parkinson’s Disease - What’s new?
There has been an extensive effort to improve surgical accuracy and efficiency over the past few years. In general, facilities have reduced operation room (OR) time, increased accuracy, improved clinical outcomes, and reduced surgical complications.
New framing systems (the device that holds your head in place during surgery) and software has eliminated the need for the painful burr holes around the skull prior to DBS implantation. New MRI and CT technology allows surgeons to have better interpretative scanning to confirm proper placement site which improves the effectiveness of the device.
INFORMED PATIENT TIP: Each facility is slightly different on their surgical techniques so it is important to ask questions about the tools utilized during surgery. Remember: New bells and whistles are nice but a well-placed lead is far more important!
DBS Option #1 - Medtronic
MRI COMPATIBILITY
Medtronic’s deep brain stimulator continues to be a strong competitor in the industry due to its compatibility with MRI scanners.
If you’re likely to have surgery in the future - a knee replacement, or back surgery, for example - you’ll likely need MRI imaging to assess those issues. Therefore, when considering a DBS system, MRI compatibility is something you must consider before making your decision as certain DBS systems such is Boston Scientific are not yet FDA approved for MRI. This does not mean they will not be in the future just currently do not have approval.
You’re able to have MRI imaging done after your Medtronic DBS system is place, however the imaging should be performed at a facility that knows the protocol and can adjust the MRI settings according. Your Medtronic representative will know these locations.
BATTERIES
Medtronic has both a primary cell and rechargeable cell option for battery use.
With a primary cell battery, you can “set it and forget it” as they typically last between 2-5 years. Once the battery life reaches a specific level, your surgeon will they switch it out by doing a quick procedure only at the battery site.
The rechargeable cell battery requires you to recharge it regularly, and can last 9-15 years depending on usage and charging frequency.
What battery is best for you? You might think about if there is any cognitive impairment that could cause the patient to forget to charge the device versus the primary you never have to think about it. In the same breathe, less surgeries overall if the rechargeable is used.
LEADS & PROGRAMMERS
Medtronic’s current leads (the wires that are inserted into your brain and connect to your battery) are omni-directional. Easiest way to explain this is when you turn a contact point on a sphere shape field of energy is formed. There is conflicting research on if directionality adds any additional clinical benefit to the patients. I will say that the industry as a whole seems to be heading more towards the directional leads.
Updates on programmers, which your healthcare provider will use to adjust the settings of your DBS, have occurred that make programming your DBS more efficient and accurate.
The new competition in the industry will most likely cause Medtronic to launch new versions of their leads and batteries in the coming years.
More Resources - Medtronic’s Deep Brain Stimulation for Parkinson’s Disease
DBS Option #2 - Abbott
MRI COMPATIBILITY
Abbott is one of the new kids on the block, and just released they have MRI compatibility with the chest placed IPGs (batteries).
BATTERIES
Abbott offers a primary cell battery at this time. This means it will last X amount of years until it will need to be replaced. They will most likely launch a rechargeable version in the next few years. Per Abbott based on how their device in made and wiring is design it has less leakage and therefore more efficient, resulting in longer battery life.
LEADS & PROGRAMMERS
Some advantages of Abbott’s lead are directionality, pulse width, and frequency. Currently in the US they offer only the primary cell battery and not a rechargeable. However, based on how the system delivers the current to the leads it is more efficient and thus may last longer.
The 2 middle contacts on Abbott’s lead are cut into 33 degree pieces that can be directed together or independently of each other. In theory, this directionality gives you better symptom control with fewer side effects, but more research is needed to fully confirm that statement.
The pulse width (another setting your HCP can manipulate) can be adjusted in great range, which can give you a larger therapeutic window to treat symptoms. In addition, frequency (another setting) can be changed for each side of the body, instead of together as Medtronics does.
Interface with the provider is wireless and does not require a remote or extension from the programming. Abbott also has a wireless update capability, meaning any new software updates can be updated directly to the battery/computer. This interface makes it easier for providers to program and easier interface for the patient to use their own remote.
More Resources - Abbott’s Deep Brain Stimulator for Parkinson’s Disease
DBS Option #3 - Boston Scientific
MRI COMPATIBILITY
Boston currently does not have MRI approval. You can have a CT or X-ray with any of the systems.
BATTERIES
Boston Scientific only offers a rechargeable device. The battery can last up to 15 years depending on recharging habits. Think of the battery similar to a phone battery. If you charge too often or let the battery run out this not good for the battery health. The recharging system is through a wireless interface with the battery that is put over the top and help in place for given period to recharge. Depending on how well you place the charger on to will determine how fast the battery charges.
LEADS & PROGRAMMERS
Similar to Abbott, Boston Scientific’s DBS has a wider pulse width capability and individualized frequencies, thanks to a concept called “fractionalization”. Fractionalization is the ability to manipulate width amplitude at each individual contact point on your brain separately.
Why does this matter to you as a patient? In general terms, it allows the practitioner who will program your DBS to be more specific and fine-tune your settings for improved symptom control.
Let me give you an example. If I set your DBS parameters to deliver 4 milliamps (mA) into the bottom two contacts of the Medtronic or Abbott systems, both contacts would deliver 4 mA. However, the Boston Scientific’s DBS lead has the ability to have 3 mA be delivered to the lower contact and 5 to the higher contact. This can be important for patients who obtain good to excellent symptom control on a particular lead but start to have a side effect at higher amplitudes. For example, if you have good tremor control when the 1st contact is set at 2 mA, but slurred speech at 2.5 mA, you want to keep the 1st contact at 2 mA. Then, you adjust the 2nd contact to 3 mA and see an additional improvement in the tremor without slurred speech. Thus, to maximize symptom control, you have the ability to have the 1st contact active at 2 mA and the 2nd contact at 3 mA.
Don’t worry if the example above is confusing to you! Your practitioner will be trained and knowledgeable about how to program your DBS for maximal results.
More Resources - Boston Scientific’s Deep Brain Stimulator for Parkinson’s Disease
So, which DBS system is the best?
There are additional technical differences in connection types, shape of batteries, elastic quality to wiring but these are the biggest clinical differences. In general, all 3 products give increased functionality and symptom control to patients.
KEY TAKEAWAY: At the end of the day, your top priority is the ability for your surgeon to achieve great placement of the leads in your brain. After that, some of these extra “bells and whistles” should be considered to improve your outcomes (ie. how well you move, how well your symptoms are controlled, etc.) after surgery.
What to do when your Deep Brain Stimulator isn’t working?
Regardless of which DBS system you choose, troubleshooting ineffective or inefficient DBS settings after surgery and beyond can be a challenge.
Each facility is uniquely different on how they adjust a patient’s DBS settings. Some facilities offer short sessions (less than 30 minutes), while others designate up to 2.5 hours for each programming session. Some facilities allow the patient to make small adjustments on their own (within parameters set by their practitioner), and others will not let you touch the device. Before surgery, ask your healthcare provider what their programming process is like and who will be involved so you can be prepared.
INFORMED PATIENT TIP: If you are not satisfied with your care, it is perfectly acceptable to seek another opinion or perspective from a different provider, even if they didn’t perform your surgery. Educating yourself as a patient, and advocating for top-level care, is critical when it comes to understanding what DBS is and is not. This ensures you get the best results from your DBS surgery. Finally, make sure your healthcare practitioners are spending the time to explain what is going on during the entire pre- and post-operative process.
Dr. Eric M. Rhoden, DPT, received his Bachelor of Science from California State University San Marcos and his Doctorate of Physical Therapy from Loma Linda University in Loma Linda, California. Eric is a certified PWR! (Parkinson’s Wellness Recovery) therapist and has specialized in the Parkinson’s population since 2014. In 2016, he began deep brain stimulation programming and has become one of the primary providers at his clinic, Neurology Solutions, to program patients with DBS using all 3 systems.